Contraceptive Counselling
Contraceptive Counselling
Contraceptive counselling provides a supportive space to discuss birth control options using clear, evidence-based information. Your OB-GYN considers your health history, lifestyle, and reproductive goals to support informed and personal choices.

What Is Contraceptive Counselling?
Contraception plays a vital role in family planning, allowing individuals and couples to decide if, and when, they want to have children. It empowers you to take control of your reproductive health, providing the freedom to pursue educational, career, and personal goals without the concern of an unplanned pregnancy.
With our patient-centred contraceptive counselling sessions, we help individuals decide on contraceptive methods, menstrual regulation goals, family planning consultation and timelines, and medical considerations. Ultimately, our goal is to work with you to give appropriate OB-GYN contraception advice.
Why Contraceptive Counselling Matters
Understanding available birth control options supports unplanned pregnancy prevention, managing menstrual cycles, and future family planning.
Careful consideration of health history also helps ensure that chosen options are suitable and medically appropriate.
All of these matters are explored during a contraceptive counselling session.
VISUAL GUIDE
Types Of Contraception
There is a wide range of methods to suit your unique family planning needs


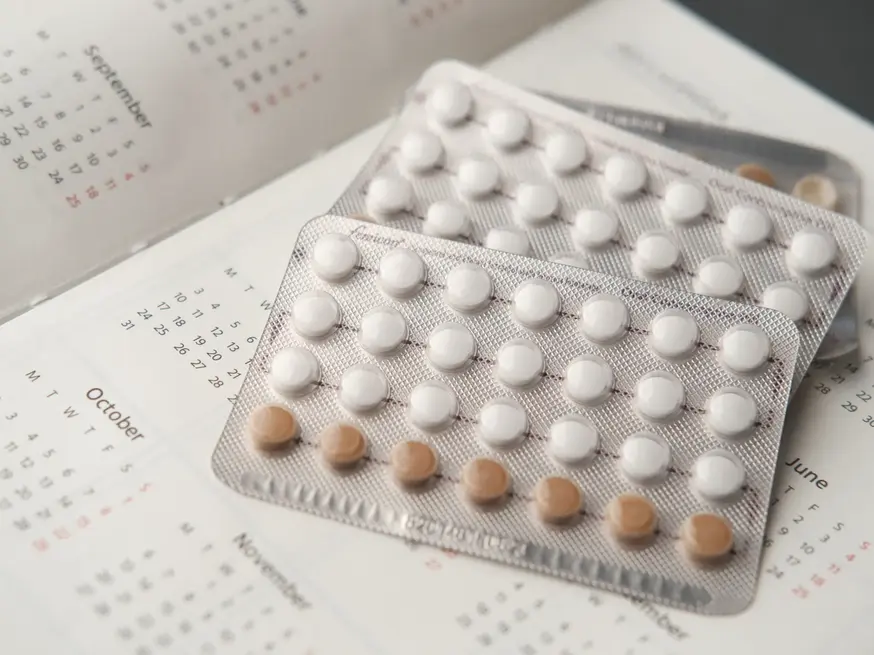
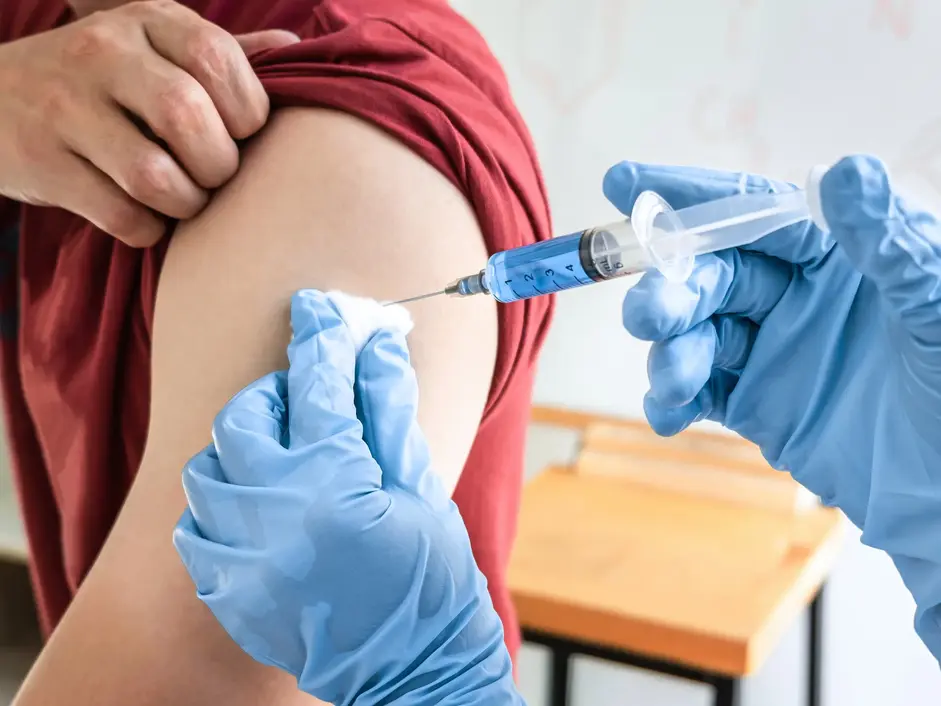



Contraceptive Options We Offer
As part of our birth control counselling services, we discuss a variety of contraceptive options to help you make informed choices that align with your needs and health considerations.
Short Term Methods:
- Oral contraceptive pills: Oral contraceptives (taken daily) contain hormones to prevent ovulation and thicken cervical mucus, making it difficult for sperm to reach the egg. Aside from pregnancy prevention, they are also chosen for their ability to aid in menstrual cycles.
- Hormonal contraceptive patch: If you do not prefer to take oral pills daily or get injections, a contraceptive patch is available. It’s a thin, adhesive patch worn on the skin(changed weekly) that releases hormones, working similarly to the oral pill.
- Hormonal injections: For those who find daily intake of pills an inconvenience, an injection(administered every 3 months), containing hormones that prevent ovulation, is an alternative.
- Condoms: Condoms are thin, flexible coverings worn over the penis or inside the vagina that help reduce the risk of sexually transmitted infections (STIs) and prevent pregnancy. They are accessible and can be used without a prescription, making them a convenient option for many.
Long-term Methods:
- Hormonal intrauterine device (IUD): A small, T-shaped device inserted into the uterus to release hormones that thin the uterus lining and thicken cervical mucus, making it difficult for sperm to reach the egg. Effective for 3-5 years.
- Non-hormonal intrauterine device (IUD): A small, T-shaped copper device inserted into the uterus, which stops the production of healthy eggs and damages sperm, preventing them from reaching the egg. Effective for 10 years.
- Birth control implant: A small, thin rod inserted under the skin of the upper arm that releases hormones to prevent ovulation and thicken cervical mucus, making it difficult for sperm to reach the egg. Effective for 3 years.
In emergencies:
- Ella: A contraceptive pill taken within 4 days of unprotected sex to inhibit/delay ovulation.
- Non-hormonal intrauterine device (IUD): Inserted within 5 days of unprotected sex to prevent embryo implantation.
Cycle & Symptom Management
Hormonal birth control can help regulate menstrual cycles, reduce heavy bleeding, and manage symptoms of conditions such as PCOS. It may also improve acne by balancing hormone levels. Method choice should be guided by individual health history and clinical advice.
Natural & Non-hormonal Options
For those who do not want implants, pills, or injections, other contraceptive options for women include natural and non-hormonal methods. These may include fertility awareness methods, such as the calendar or rhythm method, cervical mucus monitoring, and other non-hormonal contraceptives like condoms.
What to Expect During Your Consultation
- Birth control counselling includes the review of your medical history, lifestyle, and reproductive goals to understand your unique needs.
- Services for contraceptive counselling in Singapore discuss different contraceptive methods, including how they work, their effectiveness, and possible side effects.
- Guidance on the correct and consistent use of your chosen method.
- Consideration of any personal preferences, comfort levels, or concerns.
- Time for questions to ensure you feel informed and supported in your decisions.
Conditions or Concerns We Consider During Counselling
- Migraines or aura: Migraine with aura causes headaches accompanied by visual or sensory changes. Women with this condition have a higher risk of ischemic stroke, and combined oral contraceptives may further increase this risk.
- Hypertension: Some birth control pills can slightly raise blood pressure. Women with high blood pressure, especially those over 35 or who smoke, should discuss safe options with a healthcare professional.
- Breastfeeding: Breastfeeding women can use several safe birth control methods, such as IUDs, minipills, implants, barrier methods, and natural family planning. Discussing with a doctor can help identify the most appropriate contraceptive options for women.
- PCOS or hormonal imbalance: People with PCOS often use hormonal birth control as the first line of medical treatment. Forms include pills, patches, and IUDs, which all help relieve the symptoms of PCOS.
- Acne and irregular periods: Young women may present with irregular menstruation, acne, or unwanted hair growth. For those not planning pregnancy, combined oral contraceptives can help regulate periods and improve hormone balance.
- Fertility planning timelines: Fertility planning timelines refer to how soon someone plans a pregnancy. Contraceptive counselling supports informed selection of methods with consideration of how quickly fertility may return after stopping them.
Benefits of Our Contraceptive Counselling Services
- Personalised Guidance: Recommendations tailored to your health, lifestyle, and reproductive goals.
- Clear Options: Easy-to-understand explanations of all available contraceptive methods.
- Cycle Support: Assistance with managing menstrual cycles and related symptoms.
- Family Planning Consultation: Guidance for short-term and long-term reproductive goals.
- Evidence-Based Care: Safe, informed decision-making led by women’s health specialists.
FAQs
1. What happens during contraceptive counselling?
- During contraceptive counselling sessions, your doctor should review your current, future pregnancy plans and your medical history, discuss contraceptive options for women, evaluate your current health, and help you decide which birth control method is best for your goals, lifestyles, and needs.
2. Which contraceptive method is best for me?
- The best contraceptive method will depend on your health, lifestyle, reproductive goals, and any medical conditions or personal preferences. A healthcare professional can help review your options.
3. Are there side effects I should worry about?
- Side effects vary depending on the contraceptive method. For example, birth control pills may cause headaches, nausea, or breast tenderness in some women, while natural methods generally have no side effects. Talk to your doctor about what to expect with each option.
4. How soon does contraception start working?
- It depends on the method. Some, like condoms or the copper IUD, work immediately. Others, like birth control pills, patches, or injections, may take several days to become fully effective.
5. Is contraceptive counselling suitable for first-time users?
- Absolutely. First-time users can benefit from contraceptive counselling to learn about available contraceptive options, understand possible side effects, and make informed choices.
6. Can contraception help regulate my period?
- Combined oral contraceptives can support more regular menstrual cycles and ease period-related discomfort. Consultation with a doctor ensures the pill selected fits your needs and health profile.
7. What if I want a hormone-free option?
- Hormone-free options include condoms and natural methods like the calendar method. However, natural methods require accurate cycle tracking and careful use for best effectiveness.

Schedule An Appointment
All contraceptive options come with their benefits and possible side effects.
Talk to one of our gynaecologists today to discuss which option best suits your needs and preferences. We are here to support you every step of the way on your reproductive journey.

